Bariatric surgery, also known as weight loss surgery, is a procedure performed on individuals struggling with obesity. It aims to aid weight loss by altering the digestive system’s anatomy, leading to changes in appetite, metabolism, and nutrient absorption. There are several types of bariatric surgery, each with its own benefits, risks, and considerations.
Bariatric surgery is a medical intervention designed for individuals who have tried and failed to lose weight through conventional methods such as diet and exercise. It offers a solution for those facing severe obesity and related health complications. By understanding the different types of bariatric surgery available, individuals can make informed decisions about their weight loss journey.
Types of Bariatric Surgery
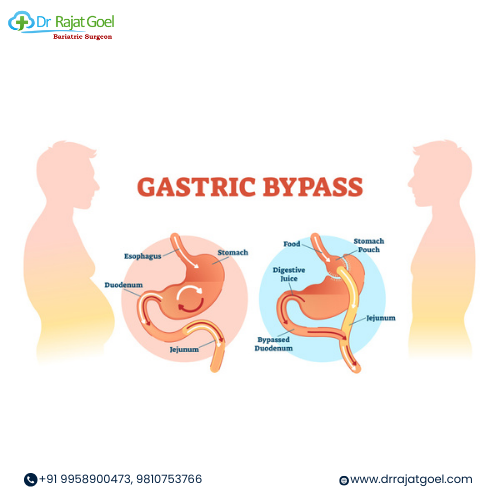
Gastric Bypass Surgery
Procedure Overview
Gastric bypass surgery involves creating a smaller stomach pouch and rerouting the digestive tract to bypass part of the small intestine. This reduces the amount of food the stomach can hold and alters the absorption of nutrients.
Benefits
Gastric bypass surgery often results in significant weight loss, improved control of obesity-related conditions such as type 2 diabetes and hypertension, and enhanced quality of life.
Risks and Considerations
Potential risks of gastric bypass surgery include infection, bleeding, nutrient deficiencies, and gastrointestinal complications. It is essential for individuals considering this procedure to discuss these risks with their healthcare provider.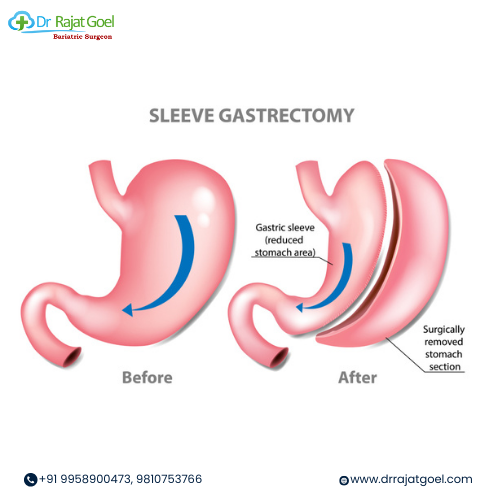
Procedure Overview
Sleeve gastrectomy involves removing a large portion of the stomach to create a smaller, banana-shaped stomach pouch. This restricts the amount of food the stomach can hold and reduces hunger-inducing hormones.
Benefits
Sleeve gastrectomy can lead to significant weight loss and improvement in obesity-related conditions. It has a lower risk of malabsorption compared to gastric bypass surgery.
Risks and Considerations
Risks associated with sleeve gastrectomy include leakage, strictures, and long-term vitamin deficiencies. Patients must follow a strict dietary plan and attend regular follow-up appointments to monitor their progress.
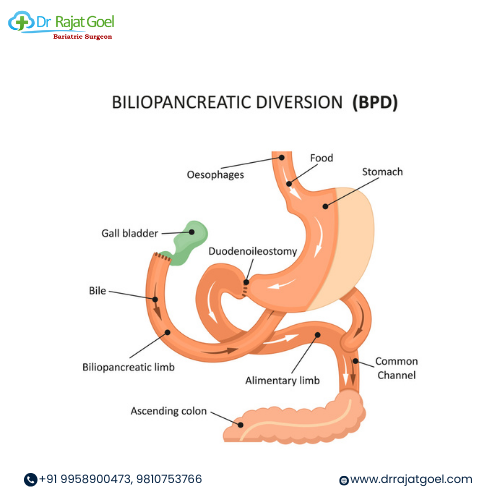
Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
Procedure Overview
BPD/DS is a complex procedure that involves removing a portion of the stomach and rerouting the digestive tract to limit food absorption. It combines restrictive and malabsorptive components for substantial weight loss.
Benefits
BPD/DS often results in rapid and significant weight loss, making it suitable for individuals with severe obesity. It can also improve or resolve obesity-related conditions such as type 2 diabetes and sleep apnea.
Risks and Considerations
BPD/DS carries a higher risk of nutritional deficiencies and gastrointestinal complications compared to other bariatric surgeries. Patients require lifelong vitamin and mineral supplementation and regular medical monitoring.
Choosing the Right Option
When considering bariatric surgery, it is crucial to weigh the benefits and risks of each procedure carefully. Factors such as BMI, medical history, lifestyle, and personal preferences should be taken into account. Consulting with a qualified healthcare provider can provide valuable guidance in selecting the most suitable option.
Life After Bariatric Surgery
Dietary Changes
Following bariatric surgery, patients must adopt a new eating plan tailored to their specific procedure. This typically involves consuming smaller, nutrient-dense meals and avoiding high-calorie, high-fat foods.
Exercise and Lifestyle Adjustments
Regular physical activity is essential for maintaining weight loss and promoting overall health. Patients are encouraged to incorporate exercise into their daily routine and adopt healthy lifestyle habits such as adequate sleep and stress management.
Monitoring and Follow-up Care
Bariatric surgery requires lifelong commitment to regular medical monitoring and follow-up care. Patients should attend scheduled appointments with their healthcare provider to track their progress, address any concerns, and make necessary adjustments to their treatment plan.
Conclusion
Bariatric surgery offers a viable solution for individuals struggling with obesity and related health issues. By understanding the different types of procedures available and their respective benefits and risks, individuals can make informed decisions about their weight loss journey. However, it is essential to remember that bariatric surgery is not a quick fix and requires ongoing commitment to lifestyle changes for long-term success.
FAQs
What is the recovery time for bariatric surgery ?
Recovery time varies depending on the type of bariatric surgery performed and individual factors. In general, patients can expect to return to normal activities within a few weeks to months after surgery.
Are there any dietary restrictions after bariatric surgery ?
Yes, patients must follow specific dietary guidelines after bariatric surgery to promote healing, prevent complications, and support weight loss. These guidelines typically include consuming small, frequent meals high in protein and low in fat and sugar.
Can bariatric surgery be reversed ?
While some procedures, such as adjustable gastric banding, may be reversible, most bariatric surgeries are considered permanent interventions. It is essential to discuss the potential reversibility of a specific procedure with a healthcare provider before undergoing surgery.
How long do the effects of bariatric surgery last?
The effects of bariatric surgery can vary depending on factors such as the type of procedure performed and individual lifestyle choices. With proper diet, exercise, and follow-up care, many patients experience long-term weight loss and improvement in obesity-related conditions.
Is bariatric surgery covered by insurance?
Insurance coverage for bariatric surgery varies depending on the individual’s policy and medical necessity criteria. It is recommended to contact the insurance provider to determine coverage eligibility and requirements.